736
Views & Citations10
Likes & Shares
Objective: Determine the
efficacy of the anterior skull base reconstruction in adult patients with
intranasal meningoceles and meningoencephaloceles treated by endoscopic
endonasal approach.
Study design: Retrospective
observational study of adult patients admitted to a tertiary hospital.
Materials and
methods: Intranasal meningocele was defined as a protrusion of meninges through a
defect in the skull base forming a cyst filled with cerebrospinal fluid in the
nasal cavity or paranasal sinuses. If the cyst had brain tissue it was called
meningoencephalocele.
The electronic clinical records of patients admitted with suspected of
intranasal MC or MEC between January 2010 and December 2018 were reviewed.
All patients treated by endoscopic endonasal approach were included. We
excluded those cases with anterior skull base previous surgeries (iatrogenic or
following tumoral resections), reconstruction with external surgical approaches
and those who were less than 18 years old.
Results: Intranasal MC was
the most frequent lesion (6/5) and there was one patient with MEC (1/6). 5
cases were idiopathic and one patient had history of transnasal surgery. A
total of 83.3% of the cases were primary surgeries and one patient had 3 prior
MC surgeries. Only in four of them (66.6%) the lesion location was detected by
at least one of the studies (CT, MRI and/or endoscopy). We performed a
multilayer closure technique in all patients. During the immediate
postoperative period, one patient had acute meningitis. One patient had a CSF
leak recurrence 4 months after surgery. The success rate of the reconstructions
performed by endonasal approach was 83.33% (5/6). The average follow-up of the
patients was 15 months.
Conclusion: The effectiveness
of the anterior skull base reconstruction in adult patients with meningoceles
and meningoencephaloceles performed by endoscopic endonasal approach in our
series was 83.33% (5/6). This procedure is currently the gold standard due to
its high efficacy and low morbidity. According to current studies, it is
recommended to perform the reconstruction with a multilayer technique.
Keywords: Skull base,
Meningocele, Meningoencephalocele, Endoscopic, Surgery
Abbreviations: MC: Meningoceles;
MEC: Meningoencephalocele
INTRODUCTION
Meningocele (MC) and meningoencephalocele (MEC) are protrusion of
meninges through a defect in the skull base forming a cyst filled with
cerebrospinal fluid in the nasal cavity or paranasal sinuses. They may have
only liquid content (cerebrospinal fluid) or brain tissue. The brain tissue
inside is usually not functional. The skull base defect can be either
congenital or acquired (intracranial hypertension, trauma, surgery, expansive
tumors, etc.). If there is no bone defect, with heterotopic brain tissue, it is
called glioma.
The incidence of congenital MC is 1 per 3,000-10,000 newborns. The
underlying mechanism may be defects of the neural tube caused by genetic
alterations (approximately 10% of the cases). Treatment of these lesions is
based on repairing the bone defect in
order to avoid
the risk of
STUDY DESIGN
Retrospective observational study of adult patients admitted to a
tertiary hospital.
OBJECTIVE
To determine the efficacy of the anterior skull base reconstruction in
adult patients with intranasal meningoceles and meningoencephaloceles treated
by endoscopic endonasal approach.
MATERIALS AND METHODS
Intranasal meningocele was defined as a protrusion of meninges through
a defect in the skull base forming a cyst filled with cerebrospinal fluid in
the nasal cavity or paranasal sinuses. If the cyst had brain tissue it was
called meningoencephalocele.
The electronic clinical records of patients admitted with suspected of
intranasal MC or MEC between January 2010 and December 2018 were reviewed.
The inclusion criteria were age>18 years, treated by endoscopic
endonasal approach. We excluded those cases with anterior skull base previous
surgeries (iatrogenic or following tumoral resections), those who had previous
reconstructions with external surgical approaches.
The electronic clinical histories were reviewed. Demographic data and
clinical characteristics were obtained. Data were retrieved by 2 independent
operators and reviewed by the principal investigator in order to detect
erroneous values and missing information. The specific data recorded were age,
sex and preexisting baseline comorbidities. We retrospectively analyzed and
compared medical records of patients diagnosed with intranasal MEC and MC. A total
of 6 patients were diagnosed with intranasal MC and 1 patient with MEC. We
excluded 1 female patient with an ethmoidal MC and history of previous
rhinoseptoplasty 7 years earlier who had suffered recurrent meningitis that
refused treatment. A total of 6 patients were included, four were women and two
men, the average age was 52 years old. In all cases we studied them by nasal
endoscopy, CT scan and MRI.
Surgeries were performed under general anesthesia. The endonasal
approach varied according to the location of the lesion. Whenever was possible,
the defect’s surrounding bone tissue was exposed by resecting the surrounding
mucosa to prepare the surgical site for the graft or flap. In all of them a
multilayer repair was made, using autologous grafts and/or flaps. Then a
synthetic adhesive was placed, followed by Spongostán and an anterior nasal
packing, left in place for 6 days.
All patients were admitted to the intensive or intermediate care unit
for an average of 7 days and received antibiotic prophylaxis treatment until
nasal packing was removed.
RESULTS
Intranasal MC was the most frequent lesion (6/5) and there was one
patient with MEC (1/6). Five cases were idiopathic and one patient had history
of transnasal surgery for a tumor of the sellar region and sphenoid plane 15
days before. 83.3% of the cases were primary surgeries and one patient had 3
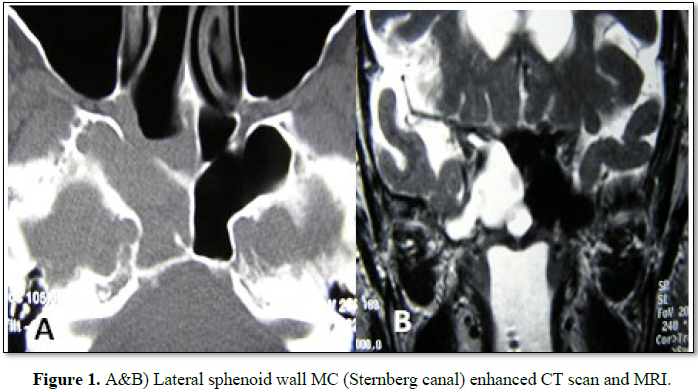
prior MC surgeries. In 2 cases the MC was located in the sphenoid lateral wall (Figures 1A and 1B), one was located in
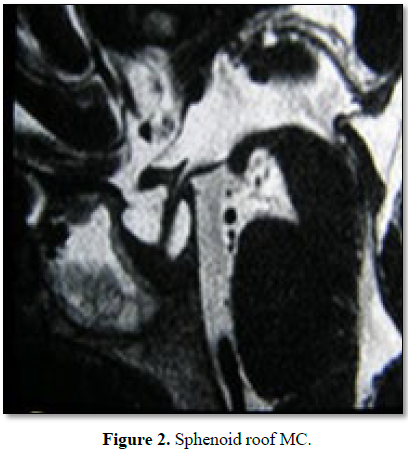
the sphenoid roof (Figure 2), 2 in
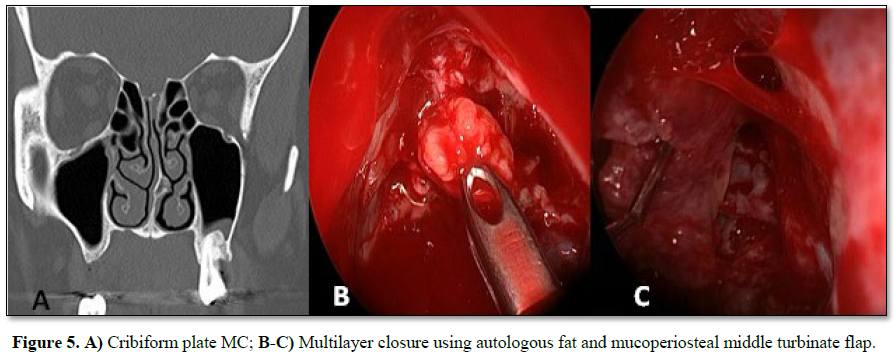
the cribriform plate and one patient, with MEC diagnosis, had it located in the
frontal sinus. 66.6% had anterior rhinorrhoea (4/6) (Table 1).
All patients were studied before surgery, only in four of them (66.6%)
the lesion location was detected by at least one of the studies (CT, MRI and/or
endoscopy). For one patient with MC of the lateral sphenoid wall intrathecal
fluorescein was used prior to surgery (10 cc of CSF were extracted by lumbar
puncture and mixed with 0.2 ml of 5% fluorescein, then 1 ml/min was delivered
by intrathecal injection.
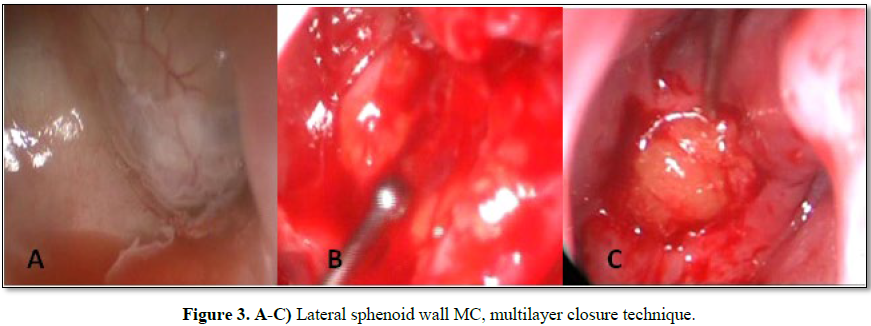
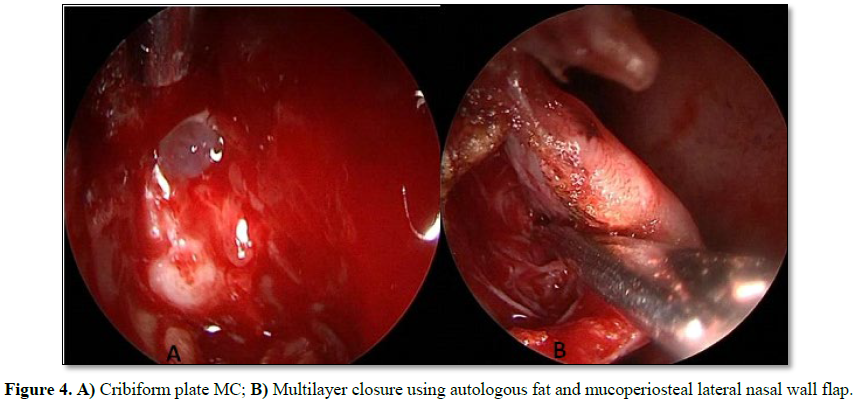
We performed a multilayer closure technique in all patients (Figures 3A-3C). In 4 cases we used
autologous fat with mucoperichondrium (Figures
4 and 5) and in 2 cases autologous cartilage with mucoperichondrium. We
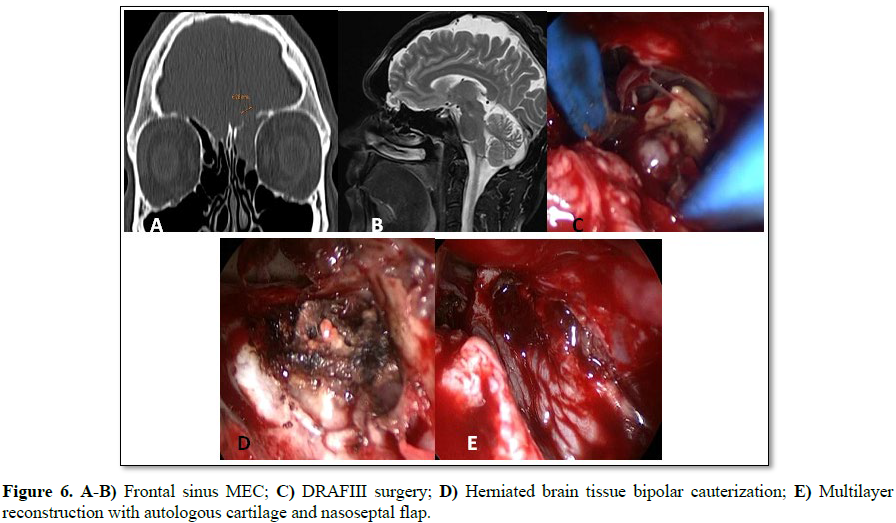
used an intranasal transpterygoid approach for one case of lateral sphenoid
wall mucocele, a Draf III technique in une case of frontal sinus MEC (Figures 6A-6E).
During the immediate postoperative period, one patient had acute
meningitis that resolved with intravenous empirical antibiotics. One patient
had a CSF leak recurrence 4 months after surgery. He was treated by external
approach and had no relapse.
No complications during postoperative follow up. The success rate of
the reconstructions performed by endonasal approach was 83.33% (5/6). The
average follow-up of the patients was 15 months.
DISCUSSION
Meningoceles (MC) are protrusion of meninges through a defect in the
skull base forming a cyst filled with cerebrospinal fluid in the nasal cavity
or paranasal sinuses and it is called meningoencephalocele (MEC) when it has
brain tissue content. These are infrequent lesions, with an incidence of
approximately 1 in 35,000 and are usually located in the anterior cranial fossa
chronic. It may be congenital, as a result of a neural tube closure abnormality
or acquired, after previous trauma or surgeries.
MC occurs more frequently in middle-aged obese women, who also tend to
have clinical symptoms and radiological signs of intracranial hypertension
(IH). Among the radiological signs, there is a high incidence of empty sella
going from 6% in the general population to 94% in patients with IH. Some of these
patients don't have the typical symptoms of this entity, since there is an
active leak of CSF and they do not develop intracranial hypertension symptoms
until their fistula has been repaired. This fact probably contributes to the
failure of long-term surgical treatment and the recurrence rate of these
patients. In our series, two female patients with sphenoid meningoceles were
obese (body mass index>30), only one had an elevated intracranial pressure
(IP). None of the patients in our series had signs or symptoms of intracranial
hypertension.
The most accepted theory to explain the development of MC establishes
its relation with intracranial hypertension secondary to a disorder of CSF
reabsorption in arachnoid granulations. Persistent elevations and significant
fluctuations in IP levels may cause the development of aberrant arachnoid
granulations, which penetrate the dura but do not drain into any venous sinus.
The pulsatility of CSF maintained over the years is able to reshape and erode
the bone. Points of low resistance are more frequent in pneumatized areas of
the skull base: cribriform plate, midline and lateral wall of the sphenoid
sinus (particularly at a point called the craniopharyngeal or Sternberg canal),
the sellar diaphragm, the tegmen timpany and the floor of the middle cranial
fossa.
The craniopharyngeal or Sternberg lateral canal is produced by the lack
of fusion of the ossifying points of the sphenoid sinus (between the greater
wings and the anterior sphenoid) during the embryonic period [2,3]. This
region, located posterolateral to the inferior wall of the sphenoid sinus, is
covered only by connective tissue, being the area of least resistance of the
skull base. This canal was described by Sternberg in 1888 for the first time 2
and is present until 3-4 years of age [4]. It is estimated that 0.1% to 4% of
adults have persistence of this canal [4]. In our series, three patients had MC
in the sphenoid sinus: one in the midline and two in the lateral wall.
Evaluation in these patients should always be with CT and contrast
enhanced MRI to assess the content of the cyst and its possible
vascularization. Patients with these pathologies have a higher risk of
meningitis, especially if there is an active CSF fistula. A CSF fistula
resolves spontaneously within the first 5 days after trauma in 80 to 90% of
patients [5]. However, the spontaneous cessation does not guarantee that the
dural tear is completely sealed, leading to recurrent rhinorrhea and deferred
intracranial infections [6]. This may be due to local clots, lacerated mucosa
and/or inflammatory tissue on the dura or brain tissue herniation. Besides, the
dura does not regenerate. In a long-term study of 160 cases of posttraumatic
CSF leak, the reported risk of meningitis before surgical treatment was 30.6%
and the cumulative risk 1.3% per day in the first two weeks, 7.4% per week in
the first month and up to 85% after 10 years of follow-up. After surgical
treatment, the risk of meningitis during the subsequent 10 years was reduced
from 85% to 7% [6].
The main objective of the treatment of MC and MEC is the closure of the
defect in the skull base to reduce risk of intracranial infections [1,7].
Compared with the external approach, it is currently considered that endoscopic
endonasal techniques are the best options to treat intranasal or sinus MC and
MEC, cause these are less invasive techniques and for its high effectiveness
[8]. The first step of the surgery is to expose the sac of the lesion and to
resect the underlying mucosa of the bone peripheral to the MC. If the content
has brain tissue it should be reduced with bipolar electrocautery, since when
it goes through a narrow hole, the brain tissue may be non-functioning. If they
are sessile and their implantation base is broad, the brain content may be
functional.
In order to achieve better outcomes, a multilayered reconstruction,
placing a graft between the skull base bone and the meninx to then cover it
with a nasal mucoperiosteal free graft or with a local pedicled flap. In cases
of MEC of the sphenoid lateral wall, some authors suggest to place overlay
grafts (covering the defect above the margins of the exposed bone), because
they consider it less invasive, having less possibilities of altering the
sensitivity of the underlying temporal lobe [9]. Abdominal fat can be used to
seal the defect in the intradural space («bath-plug technique») before the
placement of the mucosa graft [10]. All the reconstructions in our study were
performed with a multilayer technique. The autologous grafts used were septal
cartilage, rectus abdominis muscle’s fascia, mucoperiosteum of the inferior
turbinate and fat.
Martinez Arias and Manuel Bernal-Sprekelsen reviewed the literature and
found, between the year 2000 and 2014, 87 cases of MEC of the lateral wall of
the sphenoid sinus treated with endoscopic surgery. The persistence of cerebrospinal
fluid fistula was described in 6 cases. The 6 cases were repaired with complete
resolution of the fistula. The repair of the skull base failed twice in only
one case of our series (lateral sphenoid MC treated by endoscopic
transpterygoid/transsphenoidal approach). Only 2 studies used a lumbar drainage
from the time of surgery until 2 to 4 days postoperatively, despite the fact
that there was no known high intracranial pressure [11]. Castelnuovo et al.
[12] preferred not to place lumbar drainage, considering that the persistence of
some pressure at the level of the fistula is useful for the coaptation of the
“underlay” graft to the bone defect, without leaving dead spaces. Experimental
studies have shown that the graft becomes incorporated into the dura after one
week. It is essential that with any surgical reconstruction technique used,
stability of the graft or flap is ensured for the first 7 days. The
displacement of the graft is one of the most frequent causes of procedure
failure.
CONCLUSION
The effectiveness of the anterior skull base reconstruction in adult
patients with meningoceles and meningoencephaloceles performed by endoscopic
endonasal approach in our series was 83.33% (5/6). This procedure is currently
the gold standard due to its high efficacy and low morbidity. According to
current studies, it is recommended to perform the reconstruction with a
multilayer technique.
CONFLICT OF INTEREST
We declare there is no financial interest or any conflict of interest.
1.
Lai SY, Kennedy DW,
Bolger WE (2002) Sphenoid encephaloceles: Disease management and identification
of lesions within the lateral recess of the sphenoid sinus. Laryngoscope 112:
1800-1805.
2.
Al-Nashar I, Carrau R,
Herrera A, Snyderman C (2004) Endoscopic transnasal transpterygopalatine fossa
approach to the lateral recess of the sphenoid sinus. Laryngoscope 114:
528-532.
3.
Sternberg M (1888) Ein
bisher beschriebener Kanal im Keilbein des Menschen. Anat Anz 23: 784-786.
4.
Schick Β, Brors D,
Prescher A (2000) Sternberg's canal - Cause of congenital sphenoidal
meningocele. Eur Arch Otorhinolaringol 257: 430-432.
5.
Griffith HB (1990) CSF
fistula and surgeon. Br J Neurosurg 4: 369-371.
6.
Eljamel MS, Pidgeon CN,
Toland J (1994) MRI cisternography and the localization of CSF fistulae. Br J
Neurosurg 8: 433-437.
7.
Castelnuovo P, Dallan
I, Pistochini A, Battaglia P, Locatelli D, et al. (2007) Endonasal endoscopic
repair of Sternberg’s canal cerebrospinal fluid leaks. Laryngoscope 117:
345-349.
8.
Alobid I, Enseñat J, Rioja
E, Enriquez K, Viscovich L, et al. (2014) Management of cerebrospinal fluid
leaks depends on its size. Our experience. Acta Otorrinolaringol Esp.
9.
Tomazic PV, Stammberger
H (2009) Spontaneous CSF-leaks and meningoencephaloceles in sphenoid sinus by
persisting Sternberg’s canal. Rhinology 47: 369-374.
10.
Pasquini E, Sciarretta
V, Farneti G, Mazzatenta D, Modugno GC, et al. (2004) Endoscopic treatment of
encephaloceles of the lateral wall of the sphenoid sinus. Minim Invasive
Neurosurg 47: 209-213.
11.
Martínez Arias A,
Bernal-Sprekelsen M, Rioja E, Enseñat J, Prats-Galino A, et al. (2015) Abordaje
endoscópico transpterigoideo y reparación de base de cráneo tras resección de
meningoencefalocele esfenoidal. Nuestra experiencia. Acta Otorrinolaringológica
Española 66: 1-7.
12.
Castelnuovo P, Dallan
I, Pistochini A, Battaglia P, Locatelli D, et al. (2007) Endonasal endoscopic
repair of Sternberg’s canal cerebrospinal fluid leaks. Laryngoscope 117:
345-349.
QUICK LINKS
- SUBMIT MANUSCRIPT
- RECOMMEND THE JOURNAL
-
SUBSCRIBE FOR ALERTS
RELATED JOURNALS
- Journal of Infectious Diseases and Research (ISSN: 2688-6537)
- Journal of Nursing and Occupational Health (ISSN: 2640-0845)
- Journal of Ageing and Restorative Medicine (ISSN:2637-7403)
- Journal of Carcinogenesis and Mutagenesis Research (ISSN: 2643-0541)
- Chemotherapy Research Journal (ISSN:2642-0236)
- Journal of Oral Health and Dentistry (ISSN: 2638-499X)
- International Journal of Radiography Imaging & Radiation Therapy (ISSN:2642-0392)